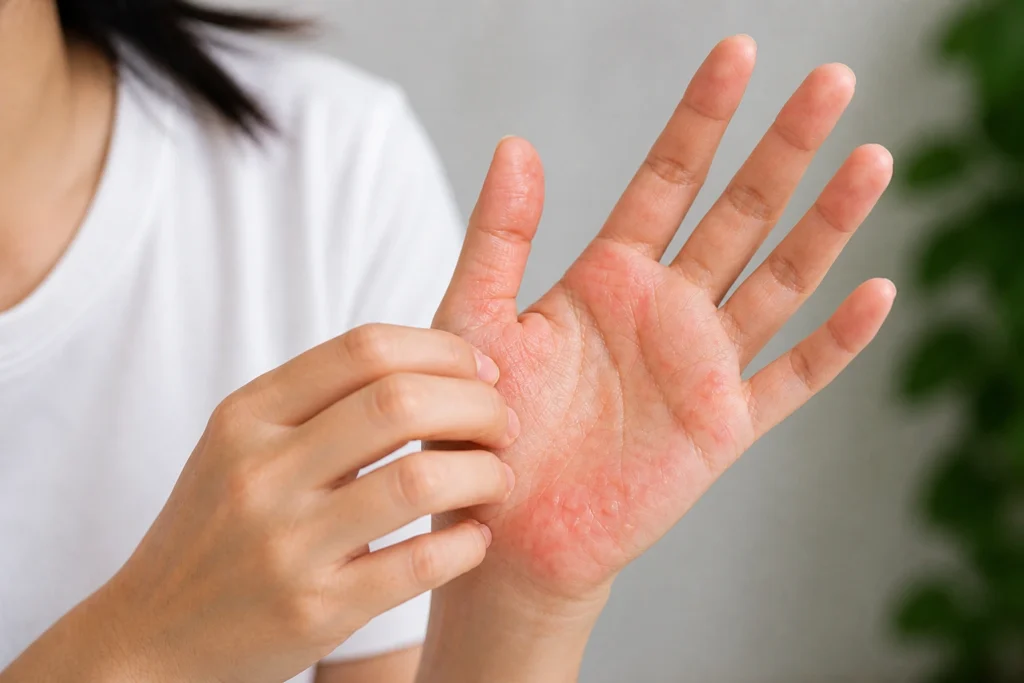
Discoid eczema causes round or oval patches of inflamed, itchy skin that can appear anywhere on the body. Unlike atopic eczema which tends to affect the creases of the body, discoid eczema shows up as distinct coin-shaped lesions, which is why it is also called nummular eczema (from the Latin word for coin).
If you have noticed well-defined circular patches of red, scaly, or weeping skin, this guide explains what discoid eczema is, what causes it, and how to manage it naturally alongside any medical treatment.
Key Takeaways
- Discoid eczema produces coin-shaped patches of inflamed skin, usually on the arms, legs, and torso
- It is more common in adults, particularly men aged 50 to 70 and women aged 15 to 30
- Common triggers include dry skin, skin injuries, harsh soaps, and nickel exposure
- Consistent moisturising is the single most important step in managing and preventing flare-ups
- Gentle, pH-balanced body wash and lotion formulated without SLS, parabens, or alcohol significantly reduce irritation
Table of Contents
- What Is Discoid Eczema?
- Discoid Eczema Symptoms
- Causes and Triggers
- How It Is Diagnosed
- Treatment Options
- Natural Skincare Management
- Daily Routine for Discoid Eczema
- When to See a Doctor
- Frequently Asked Questions
What Is Discoid Eczema?
Discoid eczema is a chronic skin condition characterised by distinct, circular or oval patches of inflamed skin. These patches can be red, swollen, crusted, or weeping, and they cause intense itching. The condition most commonly appears on the arms, lower legs, and torso, though it can develop anywhere on the body.
According to DermNet, discoid eczema affects approximately 2 in every 1,000 people. It is more prevalent in adults than children and tends to be a long-term condition that cycles between flare-ups and remission. In Malaysia, where humidity and heat stress the skin barrier daily, the condition can be particularly persistent.
How Discoid Eczema Differs From Atopic Eczema
| Feature | Discoid Eczema | Atopic Eczema |
|---|---|---|
| Patch shape | Round or oval (coin-shaped) | Irregular, diffuse |
| Location | Arms, legs, torso | Creases (elbows, knees, neck) |
| Age of onset | Adults (50 to 70 in men; 15 to 30 in women) | Often begins in childhood |
| Association with allergies | Less common | Strongly associated (asthma, hayfever) |
| Family history | Not typical | Strongly genetic |
Discoid Eczema Symptoms
Recognising discoid eczema starts with understanding how the patches typically present and evolve over time.
Early Stage
- Small, itchy spots or bumps on the skin
- Clusters of tiny blisters that may ooze clear fluid
- Redness and swelling in a defined circular area
Developed Stage
- Well-defined coin-shaped plaques, typically 1 to 10 centimetres in diameter
- Dry, scaly, or crusty surface on the patches
- Intense, persistent itch that is often worse at night
- Brown discolouration or darker patches as healing begins
Signs of Infection
Discoid eczema patches can become infected, especially when scratching breaks the skin. Signs of infection include increased redness, yellow or green crusting, warmth, and swelling beyond the patch boundary. Infected patches require medical attention rather than home management alone.
What Causes Discoid Eczema?
The exact cause of discoid eczema is not fully understood, but research points to a combination of skin barrier dysfunction, external triggers, and in some cases, previous skin injuries. A 2021 review published in the Journal of Dermatology identified dry skin and compromised barrier function as the most consistent underlying factor across discoid eczema cases.
Known Causes
- Skin injuries: Insect bites, minor cuts, or burns can trigger a patch at the injury site
- Dry skin: Severely dry skin is the most common predisposing factor
- Skin infections: Bacterial infections, particularly from Staphylococcus aureus, may trigger or worsen patches
- Certain medications: Interferon, ribavirin, and some anti-TNF therapies are linked to discoid eczema onset
- Metal sensitivity: Sensitivity to nickel (found in jewellery, belt buckles, and some foods) is associated with flare-ups in some individuals
Common Triggers in Malaysia
In Malaysia’s tropical climate, several environmental factors are especially relevant for people with discoid eczema.
- Air conditioning: Prolonged exposure strips moisture from skin, severely drying the barrier and triggering patches
- Harsh soaps and body washes: Products containing SLS (sodium lauryl sulfate) damage the skin’s acid mantle and accelerate barrier breakdown
- Hard water: Common in Malaysian homes, hard water strips the skin’s natural oils during bathing
- Synthetic fragrances: A leading contact irritant, present in most conventional body washes and detergents
- Dust mites: Present in over 85% of Malaysian homes above sensitisation thresholds, dust mites are a well-documented eczema trigger
How Discoid Eczema Is Diagnosed
Diagnosis is typically clinical, meaning a dermatologist examines the appearance, location, and pattern of the patches. There is no definitive blood test or biopsy result that confirms discoid eczema, though a skin biopsy may be performed to rule out other conditions like ringworm (tinea), psoriasis, or Bowen’s disease.
Patch testing may also be recommended to identify contact allergies, particularly to nickel or fragrances, which may be contributing to the condition.
Discoid Eczema Treatment Options
Medical Treatments
Medical treatment for discoid eczema focuses on reducing inflammation and managing the itch cycle. Your doctor may recommend:
- Topical corticosteroids: Moderate to potent strength steroids applied to active patches to reduce inflammation, typically for short courses
- Topical calcineurin inhibitors: Steroid-free alternatives such as tacrolimus for use on sensitive areas or in patients who cannot use steroids long-term
- Oral antihistamines: To manage nighttime itch and improve sleep during active flare-ups
- Oral antibiotics: If infection is present, a short course of antibiotics may be needed before other treatments can be effective
- Phototherapy (UVB): For widespread or persistent cases, narrowband UVB light therapy has evidence for reducing discoid eczema patches
None of these treatments cure discoid eczema. Long-term management requires consistent skincare to maintain the skin barrier and reduce the frequency of flare-ups.
Natural Skincare Management for Discoid Eczema
Natural management is not an alternative to medical care during active flare-ups, but it is the foundation that determines how often flares happen and how quickly patches heal. The goal is to restore and maintain the skin barrier so patches have less chance to form.
Switch to a Gentle, pH-Balanced Body Wash
Most conventional body washes have a pH of 8 to 10, which is significantly more alkaline than healthy skin (pH 5.4 to 5.9). This disrupts the acid mantle, damages barrier lipids, and promotes bacterial overgrowth, all of which worsen discoid eczema patches.
Goat milk body wash naturally mirrors skin’s pH at 6.4 to 6.8, making it one of the few cleansing options that does not strip or disrupt the barrier during washing. Clinical trials indexed on PubMed confirm that goat milk formulations reduce atopic dermatitis incidence by approximately one-third, with comparable benefit for other eczema subtypes.
Moisturise Immediately After Bathing
The three-minute rule is critical for anyone with discoid eczema: apply moisturiser within three minutes of stepping out of the shower, while the skin is still slightly damp. This traps moisture in the upper skin layers and prevents the trans-epidermal water loss that drives barrier breakdown.
A body lotion containing niacinamide, panthenol, and goat milk provides three layers of barrier support. Niacinamide stimulates ceramide production by up to 34% (Journal of Cosmetic Dermatology, 2000), ceramides being the lipid molecules that make up approximately 50% of the skin barrier. Panthenol (pro-vitamin B5) accelerates skin cell regeneration and reduces water loss. Goat milk contributes essential fatty acids including capric, caprylic, and caproic acid, which replenish the barrier’s lipid layer directly.
The Yagishi Premium Goat’s Milk Body Lotion contains all three actives, formulated without SLS, parabens, mineral oil, or alcohol. It is rated 4.82 out of 5 by verified customers, including eczema sufferers who report reduced patching, itch relief, and improved skin texture within two to four weeks of consistent use.
Avoid Known Irritants
- Switch to fragrance-free laundry detergent
- Wear loose, breathable cotton clothing over affected areas
- Avoid nickel-containing jewellery, belt buckles, and watch straps if you have identified metal sensitivity
- Use lukewarm water (not hot) for bathing and limit showers to 10 minutes
- Pat skin dry gently rather than rubbing
Daily Skincare Routine for Discoid Eczema
Morning
- Rinse face and body with cool or lukewarm water only (no second cleanse needed if you showered at night)
- Pat dry immediately
- Apply body lotion to all affected and at-risk areas while skin is damp
- Allow to absorb fully before dressing
Evening
- Shower with a pH-balanced, SLS-free, fragrance-free body wash
- Keep shower under 10 minutes, water temperature lukewarm
- Pat dry within one minute of stepping out
- Apply body lotion within three minutes of drying
- Apply any prescribed topical treatment over the lotion on active patches if directed by your doctor
When to See a Doctor
See a dermatologist or general practitioner if:
- Patches have been present for more than two weeks without improvement
- New patches are spreading rapidly or appearing in new areas
- Patches show signs of infection (yellow crusting, warmth, increased swelling)
- Nighttime itch is severe enough to disrupt sleep regularly
- Over-the-counter or home management has not reduced patch size or frequency within four weeks
In Malaysia, you can access dermatology consultations at public hospital outpatient clinics (referral required) or at private skin clinics in Klang Valley, Penang, and Johor Bahru without referral. A diagnosis takes one appointment and gives you a treatment plan to work from.
Frequently Asked Questions
Is discoid eczema contagious?
No. Discoid eczema is an inflammatory skin condition, not an infection, and it cannot be passed from person to person through skin contact. However, if patches become secondarily infected with bacteria, the infected areas should be covered to prevent spreading the bacterial infection.
What is the difference between discoid eczema and ringworm?
Both produce round patches on the skin, which can make them difficult to distinguish without a clinical examination. Ringworm (tinea corporis) is a fungal infection that typically shows a clearer centre with a raised, scaly ring border, while discoid eczema patches are uniformly inflamed throughout. Ringworm responds to antifungal treatment; discoid eczema does not. A dermatologist can confirm the diagnosis.
Can discoid eczema go away permanently?
Discoid eczema can go into long-term remission with consistent management, but it is considered a chronic condition. Many people experience no new patches for months or years when they maintain a disciplined skincare routine and avoid known triggers. Complete permanent resolution is possible in some cases, particularly in younger patients, but flare-ups can return after injury, illness, or environmental changes.
What body wash is safe for discoid eczema?
Choose a body wash that is SLS-free, SLES-free, paraben-free, fragrance-free, and pH-balanced (ideally pH 5.5 to 6.8). Goat milk body wash meets all these criteria and additionally provides lactic acid (a gentle alpha-hydroxy acid that removes dead skin without disrupting the barrier) and essential fatty acids that begin barrier repair during cleansing itself.
How long do discoid eczema patches take to heal?
With appropriate treatment and consistent moisturising, active patches typically reduce in size and itch within two to four weeks. Complete healing of the skin surface, including resolution of discolouration, may take two to three months. Post-inflammatory hyperpigmentation (darker patches where eczema was) can persist for several months after the eczema itself has cleared.
Conclusion
Discoid eczema is manageable with the right combination of medical treatment during flare-ups and consistent daily skincare to protect the skin barrier between flares. The cleansing and moisturising steps matter more than most people realise: using the wrong body wash can actively undo whatever progress your treatment is making.
For anyone dealing with discoid eczema in Malaysia, switching to a pH-balanced, SLS-free cleanser and a barrier-repairing moisturiser with niacinamide and goat milk is the most impactful change you can make outside a doctor’s office. See a dermatologist for active patches, and use your skincare routine to reduce how often those patches come back.